In today’s healthcare industry, profitability and sustainability are defined by one factor—reimbursements. Every transaction between provider and payer directly impacts revenue. The smoother these transactions are, the stronger your financial performance will be.
When claims are denied or delayed, organizations must spend additional time and resources to recover payments. In some cases, the reimbursement is never collected, resulting in a complete loss. This is why healthcare revenue cycle analytics has become a critical tool for providers who want to maximize reimbursements, minimize denials, and strengthen financial outcomes.
In this article, we’ll explore what revenue cycle analysis is, highlight key RCM metrics to monitor, and share strategies for using analytics to unlock hidden profits in your practice.

What Is Revenue Cycle Analytics?
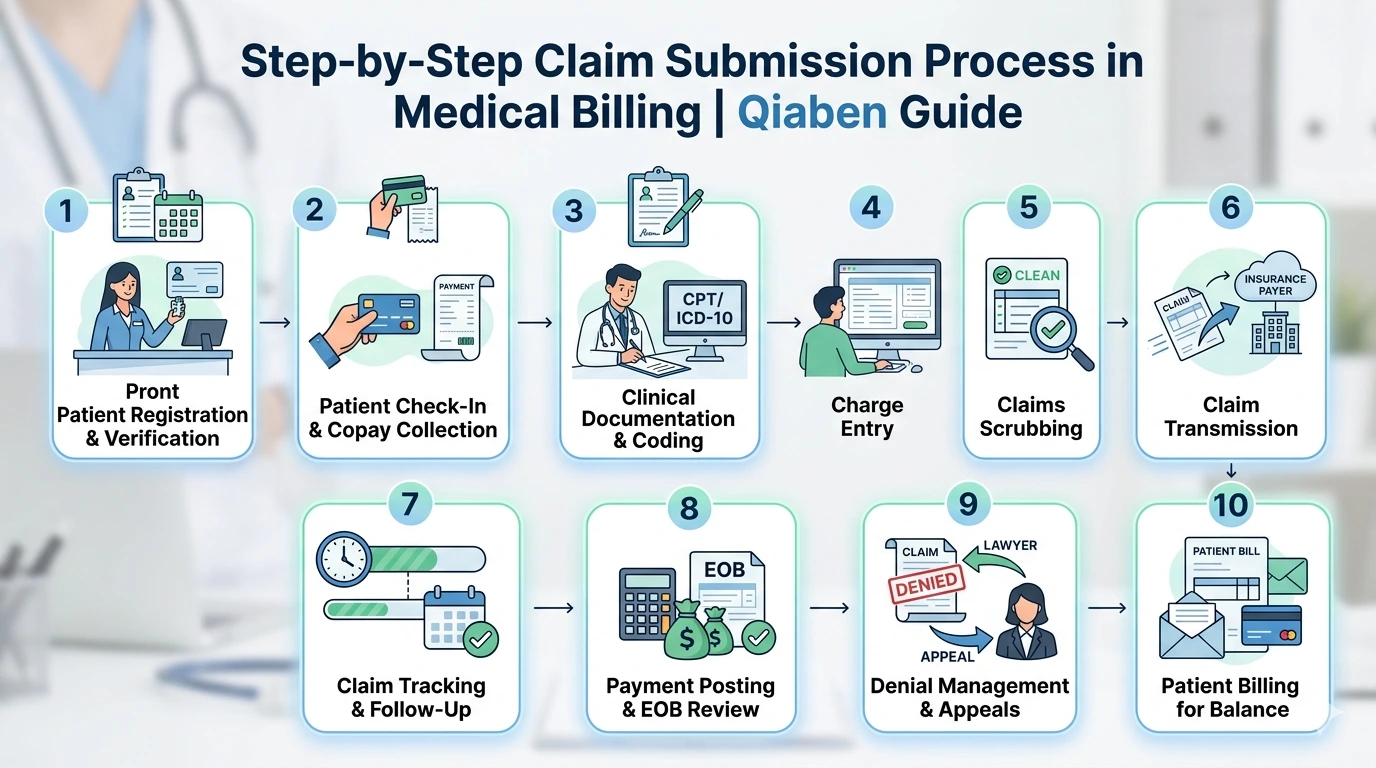
Revenue cycle analysis is the process of evaluating every step in the revenue cycle—from patient registration and eligibility verification to claims submission, payment collection, and denial management.
By taking a detailed look at these processes, healthcare organizations can identify inefficiencies, pinpoint revenue leaks, and address the root causes of claim denials. With the right improvements, providers can achieve:
Fewer denied claims
Faster payment cycles
Higher clean claims rates
Stronger financial performance
Key Metrics in Healthcare Revenue Cycle Analytics
Monitoring the right metrics is essential for making data-driven improvements. Some of the most important RCM metrics include:
Denial Rate – Percentage of claims denied on first submission.
Clean Claims Rate – Percentage of claims submitted without manual edits or corrections.
First Pass Yield – Percentage of claims reimbursed correctly on the first submission.
A/R Days – Average time it takes to receive payment from payers.
Gross Days Receivable Outstanding (GDRO) – How long it would take to collect all receivables.
These metrics provide a clear picture of how efficiently your organization is turning services into revenue.
The Importance of Revenue Cycle Analytics
Without proper analytics, healthcare providers may struggle with revenue losses. RCA plays a critical role in ensuring a steady cash flow and financial stability.
Benefits of Revenue Cycle Analytics
Faster Payments – Helps identify delays and speeds up reimbursements.
Fewer Claim Denials – Analyzes patterns to reduce claim rejections.
Increased Revenue – Pinpoints areas where revenue is lost.
Better Decision-Making – Provides real-time insights for financial strategies.
Improved Compliance – Ensures billing follows regulations.
Driving Faster Cash Flow with Analytics
Cleaner claims and fewer denials naturally lead to faster reimbursements. This not only reduces A/R days and GDRO but also makes cash flow more predictable.
Predictable cash flow empowers leaders to make smarter business decisions, allocate resources effectively, and invest in future growth—all while strengthening financial stability.
Strengthening Revenue with Cleaner Claims
Every claim error reduces the likelihood of timely and complete reimbursement. Even fixable mistakes create delays, extend A/R days, and threaten compliance with timely filing limits.
Automation plays a critical role in improving the clean claims rate. By reducing manual touchpoints, providers minimize errors, accelerate reimbursements, and stabilize cash flow. According to the CAQH Index, automating administrative transactions like claims submission could save providers and payers nearly $25 billion annually.
Unlocking Insights Behind Claim Denials
Nearly 1 in 10 claims is denied, but the key to reducing denials lies in understanding why. With advanced denial analytics, providers gain visibility into:
Specific payer trends
Common coding errors
Eligibility-related issues
Root causes of recurring denials
Instead of manually reviewing each claim, healthcare revenue cycle analytics tools automate the process, providing detailed reports and actionable insights. By addressing these root causes, organizations can significantly improve their first pass yield and reduce costly rework.
Essential Revenue Cycle Analytics Metrics to Track
To maximize revenue, healthcare providers should track key RCM performance indicators such as:
- Days in Accounts Receivable (A/R) – Measures how long it takes to receive payments.
- Claim Denial Rate – Tracks the percentage of denied claims.
- Net Collection Rate – Evaluates how much of the total revenue is collected.
- First-Pass Resolution Rate (FPRR) – Shows the percentage of claims paid without resubmission.
- Patient Payment Rate – Analyzes how effectively patient payments are collected.
Fully Optimizing RCM with Healthcare Revenue Cycle Analytics
To truly unlock hidden profits, healthcare organizations need an integrated, data-driven approach to revenue cycle management. Healthcare revenue cycle analytics platforms provide:
Claim-specific and payer-specific scorecards
Automated denial insights
Benchmark comparisons
Actionable intelligence for process improvements
Providers using advanced analytics have reported up to 40% denial reduction and a 93% first pass yield, transforming their financial outlook and operational efficiency.

Why Choose Qiaben Healthcare Solutions for Revenue Cycle Analytics?
Qiaben Healthcare Solutions provides the best revenue cycle analytics services to help healthcare providers maximize revenue and improve financial efficiency. Our data-driven solutions ensure fewer claim denials, faster reimbursements, and enhanced compliance. With our expert analytics tools and proven strategies, we help healthcare organizations unlock hidden profits and streamline their revenue cycle management.