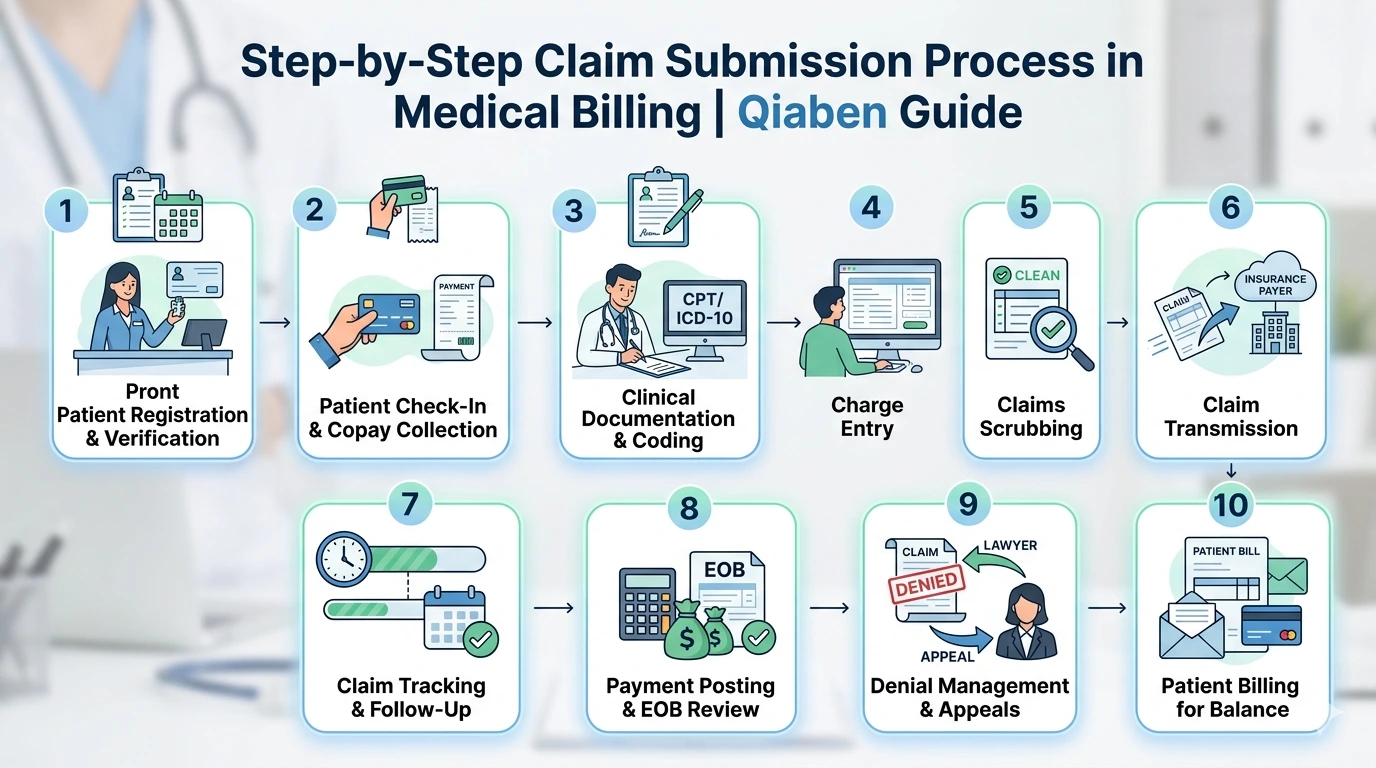
The claim submission process in medical billing is one of those things that looks simple from the outside — you see a patient, you bill the insurance, you get paid. In practice, it’s a multi-step workflow where a mistake at any point can delay payment by weeks or get the claim denied entirely.
Understanding exactly what happens at each step — and where the common failure points are — is what separates a billing team that keeps cash flow steady from one that’s constantly chasing claims. This guide walks through the full claim submission process in medical billing from the beginning of the patient encounter to the point where payment is posted and the account is closed.
Step 1: Patient Registration and Insurance Verification
This is the foundation of clean claims. Before the appointment — ideally 24–48 hours before — verify:
- Patient demographics match exactly what the insurer has on file
- Insurance ID, group number, and payer ID are current
- The policy is active and the patient is eligible
- Whether the provider is in-network for that specific plan
- Any prior authorization requirements for the planned service
- Deductible status and remaining benefits
A single transposed digit in an insurance ID number can cause a claim to reject outright. Catching it before the appointment is a five-minute fix. Catching it after a denial is a 30-minute problem.
Step 2: Patient Check-In and Copay Collection
At check-in, the front desk confirms information from verification is still accurate, collects the copay or estimated patient responsibility, and ensures a current insurance card and photo ID are on file. This is also where coordination of benefits (COB) issues should be identified.
Step 3: Clinical Documentation and Coding
After the encounter, the coder reviews the documentation and assigns:
- CPT codes — procedure codes describing what was done
- ICD-10 codes — diagnosis codes explaining why it was done
- Modifiers, where needed, to provide additional context
The diagnosis code has to support the procedure code. The claim submission process in medical billing lives and dies on coding accuracy.
Step 4: Charge Entry
Once coding is complete, charges are entered into the practice management system. Charge entry should include the date of service, place of service code, provider NPI, CPT codes with correct units, ICD-10 codes, and fee schedule amounts. Run every claim through the internal scrubber before submission.
Step 5: Claims Scrubbing
Before any claim is transmitted, it should go through a scrubbing process via the practice management system or a clearinghouse. Good clearinghouses catch:
- Duplicate claims
- Invalid or inactive provider NPIs
- Diagnosis codes that don’t match patient age or gender
- Procedure codes billed without required modifiers
- Payer-specific rules
Step 6: Claim Transmission
Once the claim is clean, it’s transmitted electronically to the payer — either directly or through the clearinghouse. Claims rejected before reaching the payer need to be corrected and resubmitted quickly.
Step 7: Claim Tracking and Follow-Up
Standard follow-up timelines:
- Commercial insurers: Follow up if no response within 30 days
- Medicare/Medicaid: Generally adjudicate within 14–30 days
- Workers’ comp and auto: Often 45–60 days before follow-up
Step 8: Payment Posting and EOB Review
When the insurer processes the claim, they send an Explanation of Benefits or Electronic Remittance Advice. Payment posting applies the payment to the correct account and identifies contractual adjustments, patient responsibility, and any denials.
Step 9: Denial Management and Appeals
Denied claims don’t mean lost revenue — they mean more work. The process involves identifying the denial reason code, determining if it’s correctable or requires appeal, correcting and resubmitting within the payer’s timely filing deadline, and writing appeals with supporting documentation.
Timely filing is non-negotiable. Most commercial payers have 90–180 day timely filing deadlines from the date of service. Missing these windows means the revenue is gone permanently.
Step 10: Patient Billing for Balance
After insurance pays, any remaining patient balance is billed to the patient. The claim submission process in medical billing wraps up when the account is balanced — either paid in full, written off per policy, or sent to collections after appropriate follow-up.
Common Failure Points
- Skipped or rushed verification — incorrect insurance info that only surfaces at denial
- Late charge entry — delays push claims close to timely filing deadlines
- No clearinghouse — claims submitted directly have higher rejection rates
- Poor AR follow-up — claims sitting unpaid past 60 days with no outreach
- Missed appeals deadlines — denials that could have been recovered but weren’t acted on
Final Thoughts
The claim submission process in medical billing is a sequence where each step depends on the one before it. A systematic audit of each stage usually reveals the problem clearly.
Qiaben works with medical and dental practices on end-to-end billing process improvement. Talk to our team if your claim submission process needs a closer look.