Dental claim denials rarely begin with the insurance company. They usually start inside the practice with small coding or documentation gaps that go unnoticed until reimbursement slows down.
If your clean claim rate is declining, accounts receivable days are increasing, or the same denial remark codes appear month after month, coding accuracy requires immediate review.
This guide explains the most common dental coding mistakes that trigger denials, outlines relevant denial codes, and provides correction strategies to protect your revenue cycle.
Why Coding Accuracy Is Critical in Dental Billing
Every CDT code submitted directly affects financial performance.
Coding accuracy impacts insurance reimbursement speed, accounts receivable aging, net collection rate, write offs and adjustments, and audit exposure.
Dental insurance carriers compare submitted codes with clinical documentation, radiographs, frequency limitations, and policy rules. When inconsistencies appear, the claim is denied, downcoded, or delayed.
Repeated coding errors gradually reduce profitability without immediate visibility.
Medically Not Necessary Denials in Dental Insurance
One of the most frequent denial categories in dental insurance billing is medically not necessary.
This denial is triggered by insufficient clinical documentation, missing radiographic evidence, lack of narrative justification, frequency limitations exceeded, or procedures that do not meet payer criteria.
Submitting a crown replacement without documenting failure of the existing restoration often results in denial.
To correct this, review payer guidelines before claim submission, attach clear radiographs and periodontal charting, provide detailed narratives explaining clinical necessity, and resubmit with complete documentation.
Prevent denials by verifying frequency limitations and medical necessity requirements during treatment planning rather than after denial.
Understanding AR Denial Codes in Dental Billing
Tracking denial codes in accounts receivable is essential for improving revenue cycle performance.
Common denial categories include eligibility denial, duplicate claim CO 18, missing attachment, incorrect CDT code, coordination of benefits issues, frequency limitation exceeded, and non covered services.
If denial codes are not categorized and reviewed monthly, patterns remain hidden and accounts receivable continues to grow.
Medical Billing Denials in a Dental Context
Although denial structures originate from medical billing, dental practices experience similar denial categories.
Eligibility denials require coverage verification before the appointment. Duplicate claim CO 18 requires confirming claim status before resubmitting. Medical necessity denials require stronger documentation and required attachments. Missing information denials require auditing claim forms before submission.
Each denial must trigger a documented corrective action to prevent recurrence.
CO 18 Denial Code Resolution
CO 18 indicates a duplicate service or duplicate claim submission.
Common causes include resubmitting claims before processing is complete, clearinghouse delays causing confusion, and incorrect secondary insurance filing.
Resolution steps include checking payer claim status online, confirming whether payment has already been issued, avoiding unnecessary resubmission, and providing the original claim control number if filing an appeal.
Duplicate submissions increase administrative workload and delay reimbursement.
Eligibility Denials in Dental Insurance Claims
Eligibility denials are highly preventable and often caused by inactive coverage, incorrect subscriber ID, wrong group number, date of birth mismatch, or coordination of benefits not updated.
Prevention depends on strong front desk processes. Insurance verification must confirm active coverage for the exact date of service.
Eligibility errors increase accounts receivable and reduce collection efficiency.
Level of Care Denials and Documentation Gaps
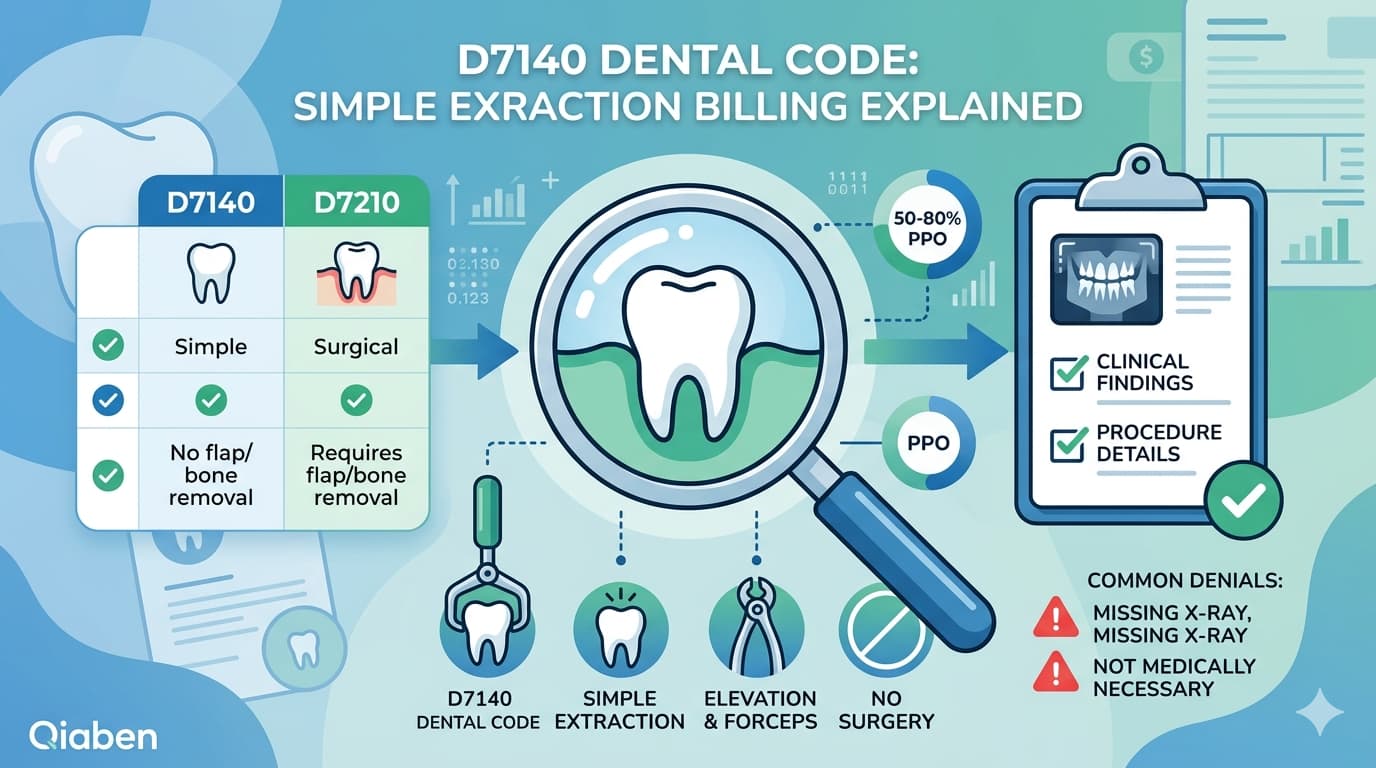
Level of care denials occur when documentation does not justify the complexity of the submitted CDT code.
Examples include submitting a surgical extraction without documenting flap creation or bone removal, or billing periodontal scaling when documentation supports only prophylaxis.
If the clinical note does not clearly support the level of service, the payer may downcode or deny the claim. Documentation must always match coding complexity.
Common Dental Coding Mistakes That Lower Clean Claim Rate
Frequent coding errors include incorrect CDT code selection, tooth number or surface mismatch between claim form and clinical chart, missing required attachments for crowns or periodontal procedures, ignoring frequency limitations, and incomplete narratives.
Each of these errors lowers clean claim rate and increases follow up workload.
Denial Remark Codes and Revenue Protection
Denial remark codes explain why payment adjustments occur.
Dental billers should review Claim Adjustment Reason Codes and Remittance Advice Remark Codes to determine whether issues involve documentation, coverage, coding, or administrative errors.
Resubmitting claims without reviewing remark codes often leads to repeated denials.
Long Term Strategies to Reduce Dental Claim Denials
Reducing denials requires structured system level improvements.
Track denial codes by payer monthly, identify the top recurring denial reasons, audit documentation for affected procedures, train providers and assistants on documentation standards, and monitor clean claim rate weekly with a target above ninety five percent.
Consistent monitoring improves net collection rate and shortens accounts receivable cycles.
Quick Self Check for Dental Coding Accuracy
Confirm radiographs are attached before submission, documentation supports every CDT code billed, eligibility checks are completed before each visit, CO 18 is not frequently appearing in accounts receivable reports, and denial remark codes are reviewed before resubmission.
If multiple concerns exist, denial volume is likely to increase.
Final Thoughts on Dental Billing and Coding Accuracy
Dental coding accuracy protects revenue. Medically unnecessary denials, eligibility rejections, duplicate claims, and documentation gaps slow reimbursement and increase operational strain.
Small improvements in coding accuracy and insurance verification processes significantly improve clean claim rate, insurance reimbursement turnaround time, accounts receivable performance, and overall revenue cycle health.
Sign Up today and start improving your revenue cycle before denial trends worsen.